
58
29
th
CONGRESS OF THE ESPU
MATERIAL AND METHODS
334 renal units with regular clinical follow-up who were treated due to VUR(vesicoureteral reflux)
between years 2009–2017 were retrospectively reviewed. Preoperative clinical parameters as
grade and laterality of reflux, presence of renal scar, initial and follow-up treatments, findings of
medical treatment and surgical procedures were analysed by grouping patients according to initial
treatment year,as before and after 2013. Clinical outcomes of surgical and medical treatments
were compared in both groups; before and after 2013. Clinical failure was identified as; performing
surgery for nonresponsive cases to medication, symptomatic urinary tract infection after surgery
and new renal scar in postoperative DMSA.
RESULTS
Mean age and follow-up duration were 71,4(6–216)months and 47(4–141)months, respectively.
We determined that VUR risk grouping does not change clinical success significantly in all risk
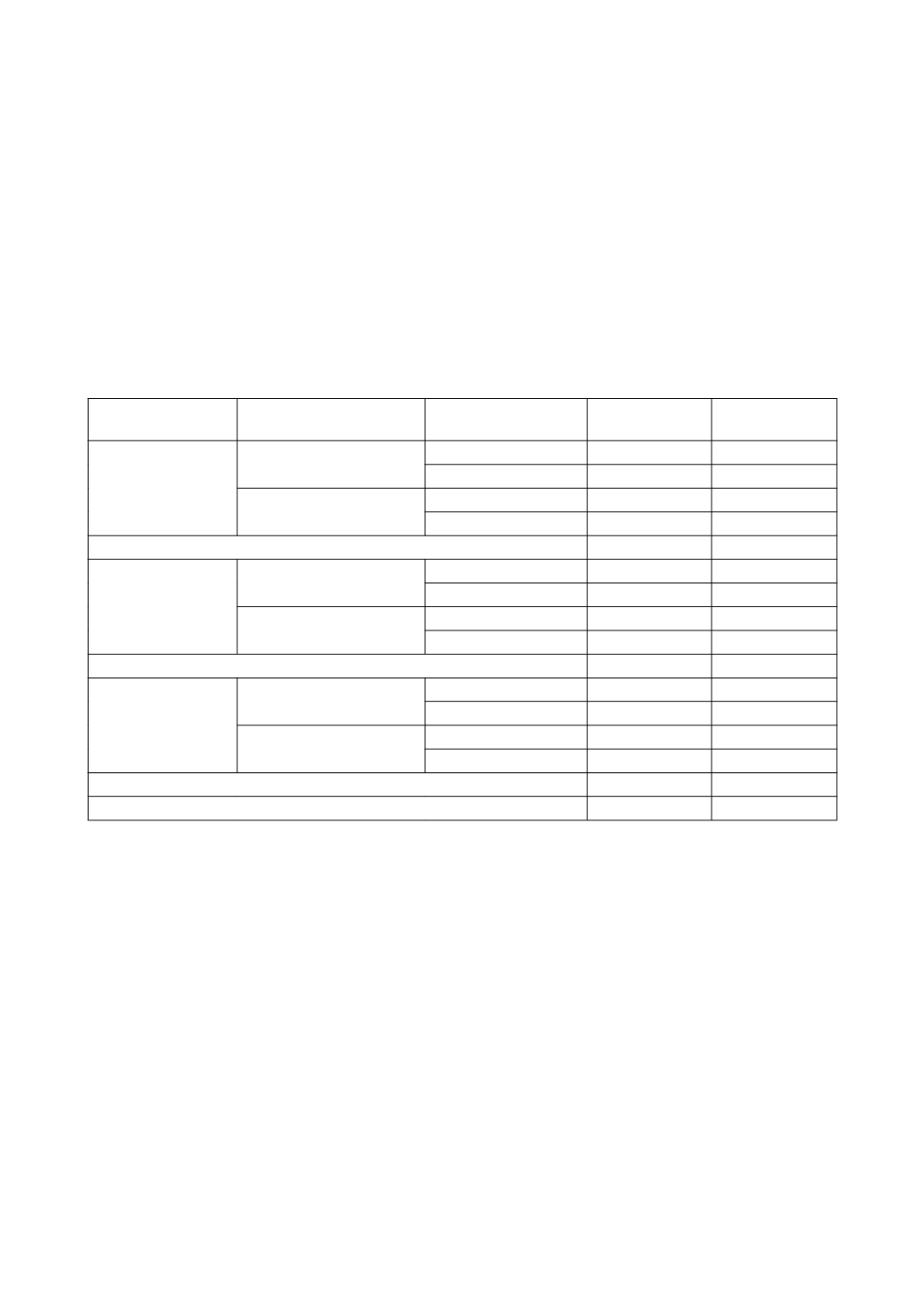
groups (table)
VUR RISK GROUP INITIAL TREATMENT
YEAR
TREATMENT
SUCCESS
MEDICAL(%)
SURGERY(%)
LOW RISK
BEFORE 2013
SUCCESSFULL
2(13)
38(93)
UNSUCCESSFULL
13(87)
3(7)
AFTER 2013
SUCCESSFULL
0
1(25)
UNSUCCESSFULL
4(100)
3(75)
p VALUE
0.4
<0.001
MODERATE RISK
BEFORE 2013
SUCCESSFULL
5(11)
95(93)
UNSUCCESSFULL
39(89)
7(7)
AFTER 2013
SUCCESSFULL
5(25)
11(78)
UNSUCCESSFULL
15(75)
3(22)
p VALUE
0.164
0.069
HIGH RISK
BEFORE 2013
SUCCESSFULL
1(5)
32(58)
UNSUCCESSFULL
19(95)
23(42)
AFTER 2013
SUCCESSFULL
0
4(67)
UNSUCCESSFULL
9(100)
2(33)
p VALUE
0.495
0.688
TOTAL
112(34)
222(66)
CONCLUSIONS
Despite the fact that EAU/ESPU VUR risk classification changed our current practice in terms
of initial treatment method, this different approach did not seem to affect early clinical success
positively. There is still an absolute need for studies with larger sample size and long-term follow-up
to reach more reliable results.
09:04–09:19
Discussion











